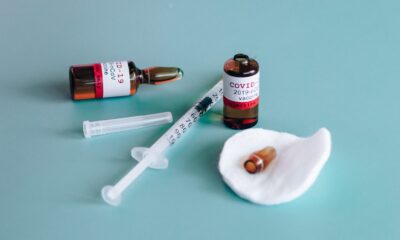
Under China’s unbending virus control policy, the country’s most populous city, Shanghai is under full lockdown. In addition, an atrocious policy in place by the ruling regime is separating young children and babies from their parents when tested positive for COVID-19.
But, what has led one of the most developed cities to the nightmare, it is living in today? How China’s Zero-COVID policy is killing thousands across the nation? And is there a way out?
Shanghai and Zero COVID Policy: The Unfolding Nightmare
On many fronts, Shanghai, one of the biggest city globally, is under a strict lockdown. Amongst the deserted market and streets, over 26 million residents are confined to their homes and breaking through the silence, the drones dictating restrictions and instructions of the locked citizens.
Shortage of food, water, and medicines, over-burdened delivery network, and growing protest to open the lockdown depict the chaotic picture of Shanghai. But, Shanghai is not alone; across China, some 23 cities, homing 200 million people are living under full or partial lockdowns.
The impact closure poses a severe impact on the Chinese economy and global supply chain. The lockdowns in the first wave of COVID led to a historic collapse in economic activities in China, and now with the Omicron lockdown, indicators are plunging again.
But, despite the draconian lockdown and security measures, new COVID cases are shooting off the roof, reflecting the high transmissibility of the mutated virus.
What is China’s Zero COVID Policy
As one of the strictest steps taken toward curbing the spread of the contagious virus, China has once again adopted the Zero COVID policy.
The matric watched the number of cases found among people who aren’t yet in quarantines. Unfortunately, this figure may continue to climb in Shanghai, and the authorities will consider an outbreak contained until the indicator known as Zero infection in society reaches zero.
The current approach tries to reduce transmission and extend the time available.
China believes that removing sick people from society is the most effective way to stop the spread of the disease. Still, quarantine facilities are divisive, producing widespread concern and terror among residents.
The primarily variant resulting in the situation is China’s low vaccination rate for the elderly, especially amongst the most vulnerable category of citizen over 80-years-old( a little over 20%). Furthermore, to add fuel to the fire vaccination campaigns have been slowing down dramatically.
How Bad is the Situation in Shanghai?
Shanghai’s local government has some special autonomy under President Xi Jinping’s China; as a province-level city, it is officially under the supervision of the central government, but it has a unique status as the country’s financial capital and an emblem of China’s accomplishments for the rest of the world.
The local administration had managed the pandemic adequately up until March, with no major breakouts. However, the quick arrival of the Omicron variety and the severe government actions accompanying it are pushing some residents to the edge.
Shanghai reported 27,719 new infections on April 14, a new record high for daily cases. But, astonishingly, 95% of these new infections are now among people in quarantine or living within a closed-loop system. The government has been testing the entire city’s population every day, and anyone who tests positive is removed from their homes and sent to centralized quarantine facilities.
The Chinese political leadership has put itself in a difficult situation by emphasizing the zero-COVID goal. If it persists, it will hamper the country’s economic recovery by exacting expenses that the people no longer consider justifiable.
However, if COVID-19 restrictions are relaxed, illnesses and fatalities will skyrocket as the virus spreads across a population lacking the protection observed in most other comparable nations.
When Will the Lockdowns End?
Once the zero COVID is achieved, Shanghai can start reopening the city. There is no timetable on when this can be achieved; however, with the new cases rising every day, it is most likely that the nightmarish lockdowns can continue for several more weeks.
Also Read: End of the Pandemic: Can We Live with COVID?
But, people are frustrated, mentally exhausted, and begging to get out. For many, this ordeal will shift how they view China as the future. While different variants of COVID killed millions around the globe, China remained a safe haven.
But, now the tables have turned.
The Urgent Needs for a Dynamic Zero-COVID Policy
Though the Chinese authorities will ultimately get the situation in Shanghai and around the country under control, the collateral damage created by the rigorous lockdown much outweighs the actual deaths inflicted by COVID at the moment.
As more cities in China sweep under lockdown, the country may again be cut off from both the inside and the outside. Moreover, what residents have gone through for the past few weeks can negatively impact their physical and mental health. As a result, the government must likewise place a premium on citizens’ mental and physical well-being.
The most vulnerable individuals should be vaccinated first, and strong safety measures should be put in place to allow regular life to continue in the state. Without these changes, the country’s economy would plummet, local firms would be forced to close, unemployment will soar, and public opinion will shift.
As a result, it’s critical to implement a dynamic zero-COVID policy that allows residents to normally go about their daily lives.



 Featured7 months ago
Featured7 months ago


 Featured6 months ago
Featured6 months ago


 Featured4 years ago
Featured4 years ago

 Featured3 years ago
Featured3 years ago


 Featured1 year ago
Featured1 year ago


 Featured2 years ago
Featured2 years ago


 Featured3 years ago
Featured3 years ago


 Featured4 years ago
Featured4 years ago